Uveitis is a common cause of blindness in horses, but in some ways it remains mysterious. In its recurrent form, it also can be intractable. There’s no cure for it yet, but it also need not be a death sentence for a horse. Careful management and treatment can help preserve a horse’s sight longer, and even in cases where an affected eye has to be removed, many horses can still continue to live largely normal, active lives and even have successful competitive careers.

Uveitis is inflammation of the eye’s uveal tract, a layer of tissue that lies between the eye’s outer layer (including the cornea) and its inner layer (the retina) and includes the iris, the ciliary body, and the choroid. This tissue is delicate, and when it’s inflamed, the effects can be painful.
“The iris sphincter muscle contracts and causes the pupil to close, so you get a constricted pupil,” explained Dr. Rana Bozorgmanesh of Hagyard Equine Medical Institute. “The ciliary body muscles spasm, and that’s pretty painful. And the blood capillaries in those areas also become leaky, and that releases proteins and cells, which results in the signs that we see.”
Those signs can include squinting, tearing, light sensitivity, a swollen or red eye, and/or a cloudy appearance or bluish haze over the cornea. The white of the eye might appear bloodshot or you might see pus or yellow deposits under the cornea in the eye’s anterior chamber. But there are also subclinical cases that might show only subtle symptoms.
“You can basically have a smoldering uveitis going on without you knowing, with tiny changes taking place in the eye until it reaches a threshold and the eye goes blind,” Bozorgmanesh said. “Often horse owners wouldn’t know the disease was there until the horse is blind in those cases. Alternatively, in other cases you will see the obvious clinical signs in the active phases of the disease.”
Causes of Uveitis
Uveitis can occur as a one-off event—caused by trauma to the eye, for example—that might never happen again and might not create future problems. But in the chronic, repeating form known as equine recurrent uveitis (ERU) or moon blindness, the disease can lead to permanent damage and eventually blindness—and it’s this manifestation that horse owners particularly worry about.
“Equine recurrent uveitis is the leading cause of blindness in horses, and it’s a progressive condition,” Bozorgmanesh said. The prevalence varies some according to a horse’s breed and geographical location, but, generally speaking, in the United States between 2% and 25% of the equine population is affected. “It’s much more prevalent in appaloosa horses; they’re genetically predisposed and have up to 25% prevalence,” Bozorgmanesh said. “German warmbloods may also have a heritable form. So it’s seen more commonly in warmbloods, draft horses and appaloosas generally as well as some quarter horses, also.”
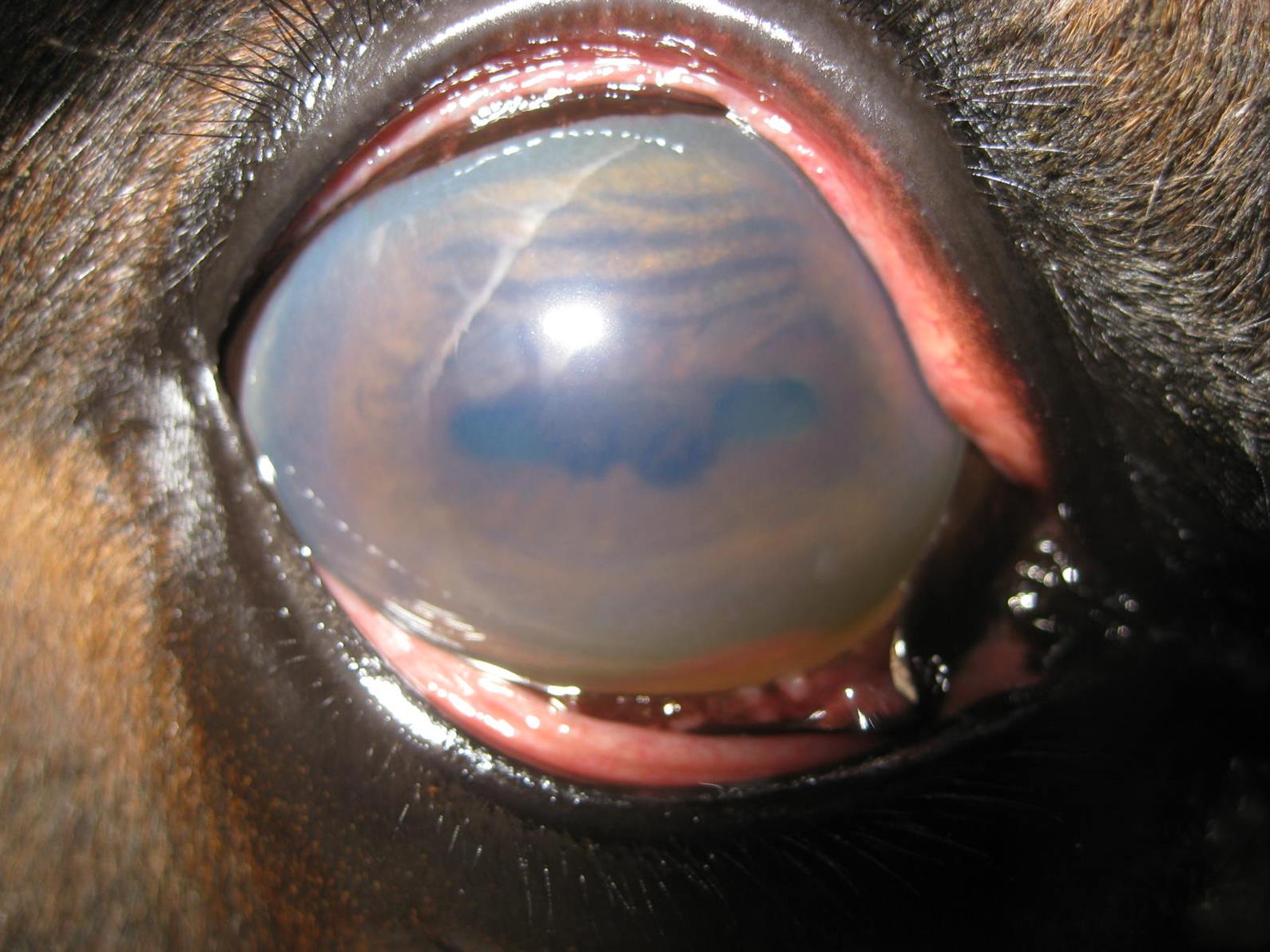
Photo: Courtesy of Dr. Rana Bozorgmanesh
and Dr. Nathan Slovis
The uveitis most commonly seen in the United States is a panuveitis, which tends to affect the front part of the eye more. In Europe, posterior uveitis—which affects the back of the eye, including the retina—is more common, but it also can be seen in the U.S.
“So people who import warmbloods into the U.S. might see a different type of uveitis,” Bozorgmanesh said.
ERU has been around for a long time.
“Recurrent uveitis used to be called ‘moon blindness,’ a term that was coined around the 1600s,” Bozorgmanesh explained. “Even back then, they noticed that horses had these recurring episodes of eye issues or what they thought was temporary blindness. At the time, they thought it was related to phases of the moon. Obviously, that isn’t the case, but it does kind of wax and wane.”
Although horse owners have been aware of the disease for centuries, its cause is still somewhat obscure.
“It’s essentially an autoimmune syndrome that has been associated with leptospirosis as the inciting cause in some cases, although that’s not 100% true of every case, or it may just be that we haven’t been able to identify leptospirosis in every case,” Bozorgmanesh said. “So the exact cause of the disease has yet to be discovered. There is a genetic predisposition—for example, in the appaloosa, it’s correlated with their coat patterns. The genetic predisposition affects the immune system, as well. So if you are genetically predisposed to having a certain kind of immune response, then if you get a certain trigger such as leptospirosis, this can result in equine recurrent uveitis.”
What to Do if You Suspect Uveitis
Your first step: call your veterinarian immediately.
“It’s important to distinguish uveitis from recurrent uveitis,” Bozorgmanesh said. “There’s no one test to figure out whether it’s ERU or just a single episode. You need your veterinarian to come out, firstly to rule out a primary cause of the uveitis, such as infection, an eye ulcer, trauma, all of those things that might be the primary reason why the horse has developed uveitis. It’s better for you and your horse if there is a clear reason that the horse has developed uveitis. If it’s just uveitis by itself, that’s more concerning, because that’s a case that could develop into recurrent uveitis.”
Because equine recurrent uveitis is progressive and does not currently have a cure, most horses that have it eventually will go blind in the affected eye.
“There are ways of slowing the progression, and with cases that we’ve been able to follow up on, we’ve had reasonable success,” Bozorgmanesh said. “But, unfortunately, because there is no cure, over the long-term, most of them are going to go blind. The prognosis is also worse if the ERU is leptospirosis-associated. Studies have shown that in cases where there’s evidence that leptospirosis has triggered their ERU, those are more likely to go blind.”
Treatment Options
There are a number of treatments available to help slow ERU’s progression.
“Even if it’s just a one-off case, you’ll be treating the horse for several weeks,” said Bozorgmanesh. “So be prepared for that.”

Photo: Courtesy of Dr. Rana Bozorgmanesh
and Dr. Nathan Slovis
The goals for treatment are to reduce the inflammation, control pain, minimize the inflammatory mediators that are promoting the inflammatory reaction, and then re-establishing the blood-ocular barrier—in other words, improve the leaks from blood vessels that are releasing cells into the eye.
Treatment options generally include topical and/or systemic non-steroidal anti-inflammatories (like Banamine); corticosteroids, which also are anti-inflammatory; and medications to dilate the pupil, which will help reduce pain. If there’s a concern that the horse has a leptospirosis infection, your veterinarian also might prescribe a two- to four-week course of antibiotics such as doxycycline or minocycline.
A device called a subpalpebral lavage catheter also can make treatment easier. The lavage system includes a port attached to the horse’s mane at the base of the neck that’s attached to a long tube that a veterinarian inserts through the horse’s eyelid. The user simply injects medication into the port, and from there the medicine is carried through the tube and directly onto the eye’s surface. The downside: the catheter can’t stay in the horse’s eye indefinitely, although it can stay in place for weeks to months if needed.
“There are also immuno-modulatory medications you can use to try to suppress the immune reaction going on in the eye,” Bozorgmanesh said. “One of those is cyclosporine, which you can sometimes use as an ointment in the eye.”
For ERU cases, cyclosporine (specifically, cyclosporine A) also can be administered through a sustained-release device—a disk implanted surgically in the eye.
“It’s not always easy to get medication into your horse’s eye,” Bozorgmanesh said. “It depends on your horse, obviously, but often in these cases you’ll be doing it up to four times a day. That’s hard work for you, and it’s something some horses won’t tolerate well. And their upper eyelid muscles are some of the strongest eyelid muscles out there! So if they don’t want you to put it in their eye, you’re not going to be able to do it. The implant helps to eliminate that work.”
A cyclosporine A implant is effective for four years or longer, which also can be more cost-effective over the long term.

Photo: bmf-foto.de/AdobeStock
“It’s a surgical procedure done under general anesthesia,” Bozorgmanesh said of the implantation. “You want a healthy horse to do that. The eye also has to be ‘quiet,’ so you can’t do the surgery if there’s a huge flare-up of uveitis underway. You have to treat the eye until the uveitis is better and quiet, and then you can place the implant.”
In cases where the implant works, Bozorgmanesh said, it has been shown to decrease the recurrence of uveitis. It also has been shown to decrease the severity and length of each episode. And it improves response to treatment in cases that still require topical treatment in addition to the implant.
For cases of posterior uveitis as sometimes seen with horses imported from Europe, there’s another surgical procedure: removal of the vitreous humor (the fluid in the back of the eye). “In this kind of uveitis, by removing that fluid you’re removing the immune mediators, the inflammatory debris—basically, everything that’s driving that immune response,” Bozorgmanesh said.
“That procedure isn’t thought to help with the more typical panuveitis we see here in the States,” she added.
Before You Treat
Because uveitis treatments like corticosteroids will suppress the eye’s immune response, it’s important to be certain before treatment that your horse doesn’t have an infection or an ulcer that might be made worse by the treatment, Bozorgmanesh cautioned.
“Otherwise the treatment might make things 100 times worse,” she said. “While you are treating with a steroid, you need to have your vet regularly check the eye. You also need to be aware that if at any point the eye suddenly looks more painful, that may be a sign that they’ve developed an ulcer or something along those lines that requires immediate attention. In that case, you need to stop the steroid immediately.
“I always tell people that just because you have a tube of eye ointment in your first-aid kit, don’t just grab it and apply it if your horse’s eye looks painful,” she added. “Different conditions require different medications.”
Removing an Affected Eye
Horse owners might also consider removing an affected eye.
“There’s not necessarily a right or a wrong when it comes to that,” Bozorgmanesh said. “ERU is a painful condition for your horse, and it is challenging for both you and the horse. You have to gauge whether removing the eye is best for you and your horse. Every case is individual. If you think your horse is suffering from the pain and you’re not able to control the pain and the flare-ups or if you physically can’t get the medication into the eye as frequently as you need to, removing the eye might be the right thing to do at a certain point.”
If you do opt for surgical removal of the eye, it doesn’t necessarily mean an end to your horse’s activity or even to his competitive career. “Horses adapt very quickly,” Bozorgmanesh said. “It’s nothing to be afraid of. There are a lot of horses out there living happy lives with only one eye, and they can still do a lot. For the majority of horses, the advantages to having a life without pain far outweigh the aesthetic advantage of having an eye that is painful.”

